Chronic Obstructive Pulmonary Disease1 , or COPD, refers to a group of diseases that cause airflow blockage and breathing-related problems. It includes emphysema, chronic bronchitis, and in some cases asthma.
A report published by the COPD Foundation2 shows that the prevalence of comorbidities is higher in COPD patients than the general population. The term “comorbidity3 ” describes two or more disorders or illnesses occurring in the same person. Comorbidities, including congestive heart failure (CHF), chronic kidney disease (CKD), diabetes, and obstructive sleep apnea (OSA) have been linked to mortality in COPD. Specific comorbidities including gastroesophageal reflux disease (GERD), CHF, diabetes, obesity, asthma and coronary heart disease (CHD) have also been associated with worse quality of life, exercise capacity, exacerbation risk and dyspnea. However, these findings have been shown for individual comorbidities, without regard to multimorbidity of the COPD population.
African-Americans (AAs) with COPD have an increased risk of mortality and experience worse quality of life than non-Hispanic whites (NHWs). In general cohorts, AAs have also been shown to have increased prevalence of and mortality from chronic conditions, such as cardiovascular disease, CKD, diabetes, and stroke.
What causes COPD?
In the United States, tobacco smoke is a critical factor in the development and progression of COPD, although exposure to air pollutants in the home and workplace, genetic factors, and respiratory infections also play a role. In the developing world, indoor air quality is thought to play a more significant role in the development and progression of COPD than it does in the United States.
Who has COPD?
Chronic lower respiratory disease, primarily COPD, was the third leading cause of death in the United States in 2014. Almost 15.7 million Americans (6.4%) reported that they had been diagnosed with COPD. More than 50% of adults with low pulmonary function were not aware that they had COPD so that the actual number may be higher. The following groups were more likely to report COPD in 2013.
- People aged 65–74 years and ≥ 75 years.
- American Indian/Alaska Natives and multiracial non-Hispanics.
- Women.
- Individuals who were unemployed, retired, or unable to work.
- Individuals with less than a high school education.
- Individuals who were divorced, widowed or separated.
- Current or former smokers.
- People with a history of asthma.
What are the complications or effects of COPD?

Compared to adults without COPD, adults with COPD are more likely to
- Have activity limitations such as difficulty walking or climbing stairs.
- Be unable to work.
- Need special equipment such as portable oxygen tanks.
- Not engage in social activities such as eating out, going to places of worship, going to group events, or getting together with friends or neighbors.
- Have increased confusion or memory loss.
- Have more emergency room visits or overnight hospital stays.
- Have other chronic diseases such as arthritis, congestive heart failure, diabetes, coronary heart disease, stroke, or asthma.
- Have depression or other mental or emotional conditions.
- Report a fair or poor health status.
How can COPD be prevented?
Avoid inhaling tobacco smoke, home, and workplace air pollutants, and respiratory infections to prevent developing COPD. Early detection of COPD might change its course and progress. A simple test, called spirometry, can be used to measure pulmonary—or lung—function and detect COPD in anyone with breathing problems.
How is COPD treated?
Treatment of COPD requires a careful and thorough evaluation by a physician. COPD treatment can alleviate symptoms, decrease the frequency and severity of exacerbations, and increase exercise tolerance. For those who smoke, the most important aspect of treatment is smoking cessation. Avoiding tobacco smoke and removing other air pollutants from the patient’s home or workplace are also important. Symptoms such as coughing or wheezing can be treated with medication. Pulmonary rehabilitation is an individualized treatment program that teaches COPD management strategies to increase the quality of life. Plans may include breathing strategies, energy-conserving techniques, exercise training, and nutritional counseling. Lung infections can cause severe problems in people with COPD. Certain vaccines, such as flu and pneumococcal vaccines, are especially important for people with COPD. Learn more about vaccination recommendations4 . Respiratory infections should be treated with antibiotics, if appropriate. Patients who have low blood oxygen levels are often given supplemental oxygen.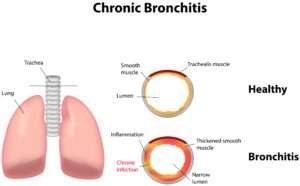
6 Tips For Talking to Loved ones about COPD5
- Know what to look for to recognize the signs of COPD in your loved one. Shortness of breath, wheezing or a chronic cough could all be symptoms of COPD, a serious but treatable lung disease.
- Talk with your loved one about things they may be missing out on, such as taking walks and playing with grandchildren, because of these symptoms.
- Talk with them about how hard daily tasks like climbing stairs and grocery shopping have become for them and that this may be related to COPD.
- Encourage your loved one to schedule a visit with their doctor or healthcare provider. COPD can be diagnosed with a simple breathing test called spirometry. It’s quick and painless – and worth it.
- Once diagnosed with COPD, there are many ways that your loved one and their provider can work together to manage the symptoms of the disease. Remind them that the earlier a person receives treatment, the better their chances to improve quality of life.
- Offer resources to help your loved one. Read through the National Heart, Lung, and Blood Institute’s COPD Learn More Breathe Better campaign Web site6 with them to learn more about COPD and support group opportunities in their area.
Enjoyed this post? Share it and read more here. Jay Harold has put together a Resource page that you may find useful when trying to improve your health and wealth. Please take this advice of Muhammad Ali and give back to others. “Service to others is the rent you pay for your room here on earth.”
Bibliography
- https://www.cdc.gov/copd/index.html
- https://journal.copdfoundation.org/jcopdf/id/1028/Comorbidities-of-COPD-Have-a-Major-Impact-on-Clinical-Outcomes-Particularly-in-African-Americans
- https://www.drugabuse.gov/publications/drugfacts/comorbidity-addiction-other-mental-disorders
- https://www.cdc.gov/vaccines/adults/rec-vac/health-conditions/lung-disease.html
- https://www.nhlbi.nih.gov/health/educational/copd/event-listing/awareness-month/pdfs/2010_Fall_LMBB_COPD_Tip_List.pdf
- https://www.nhlbi.nih.gov/health/educational/copd/index.htm